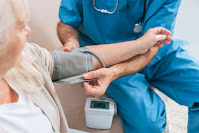
Screening cancer patients for anxiety, depression, and other symptoms of distress may help identify those at heightened risk of nonfatal self-injury, suggests a report in JAMA Oncology.
Cancer patients who scored higher on the Edmonton Symptom Assessment System (ESAS)—a tool that asks patients to score the severity of their symptoms of nausea, pain, depression, well-being, and more—were more likely to experience nonfatal self-injury within six months than those who scored lower on the ESAS.
“Nonfatal self-injury is a … manifestation of severe distress occurring in 3 out of 1,000 patients after cancer diagnosis,” wrote Julie Hallet, M.D., M.Sc., of the University of Toronto and colleagues.
To determine if routine symptom screening of cancer patients might provide clues about those at greatest risk of self-injury, Hallet and colleagues relied on data collected from adults insured through the Ontario Health Insurance Plan (OHIP). The researchers specifically focused on adults aged 18 years and older who were diagnosed with cancer between January 1, 2007, and March 31, 2019, and completed an ESAS assessment within 36 months of their cancer diagnosis.
A total of 806,910 patients, including 408,858 reporting one or more ESAS scores within 36 months of their cancer diagnosis, were included in the analysis; 753 of these patients had a nonfatal self-injury (an emergency department visit with a self-injury of intentional or undetermined intent), including 425 patients who had a recorded ESAS score up to six months prior to the injury.
The researchers compared the ESAS scores of 406 patients who experienced a nonfatal self-injury after their cancer diagnosis with 1,624 patients with cancer who did not experience a nonfatal self-injury. This comparison included how patients scored the nine individual symptoms listed on the ESAS (on a scale of 0 to 10, with 10 being worst) as well as the sum of the individual symptoms together (range: 0 to 90). The researchers defined all symptoms as moderate to severe for patients who scored 4 or higher, except for depression; moderate to severe depression symptoms were defined as a score of 2 or higher.
A higher proportion of patients with nonfatal self-injury reported moderate to severe symptoms on the ESAS than patients without nonfatal self-injury, the authors reported. “The largest absolute differences were observed for anxiety, depression, drowsiness, tiredness, and lack of well-being,” they wrote. These patients also reported higher total scores on the ESAS. Additional analysis revealed that for each increase of 10 points in a patient’s total ESAS score, there was a 51% increase in the odds of nonfatal self-injury in the following 180 days, they added.
“Effective interventions exist to prevent [nonfatal self-injury] in patients with cancer, including psychotherapy, pharmacotherapy, integrated collaborative care, muscle relaxation, therapeutic walking, and alternative cancer treatment. Support can be implemented via protocols and pathways for integrated psychosocial assessment and interventions triggered when identifying high-risk patients,” Hallet and colleagues wrote. The findings of the study suggest that patients with “moderate to severe anxiety, depression, or shortness of breath or a high [total ESAS] score should be flagged by screening programs and targeted for psychosocial evaluation, support, and longitudinal follow-up.”
For related information, see the Psychiatric News article “Expert’s Corner: Best Practices for Treating Cancer Patients With Psychiatric Symptoms.”
(Image: iStock/Ridofranz)
Did You Fail to File Report on Provider Relief Funds You Received?
The Health Resources and Services Administration has announced that health care providers who received funds from the Provider Relief Fund program and did not submit their Reporting Period 1 report by the deadline may request to submit a late report, via a DocuSign form, if certain extenuating circumstances exist. The requests must be filed from Monday, April 11, to Friday, April 22, at 11:59 p.m. ET and must attest to a clear, concise explanation regarding the extenuating circumstance; no supporting documentation is required. Those whose request is approved will be notified to complete the Reporting Period 1 report within 10 days. Providers will also have an opportunity to submit a Request to Report Late Due to Extenuating Circumstances for Reporting Period 2. Notification regarding the process to submit the request will be announced in the coming weeks. For more information, call the Provider Support Line at (866) 569-3522; for TTY dial 711. Hours of operation are weekdays from 8 a.m. to 10 p.m. Central Time.